Any excess weight promotes the development of osteoarthritis mainly, but not exclusively, in the weight-bearing joints. Conversely, patients with osteoarthritis with too much excess weight are well advised to change their diet and get a little exercise. Weight loss, even very moderate, significantly improves their functional condition while minimising painful problems.
Excess weight and obesity: a worrying situation
It is often said of people carrying too much weight that they are overweight or obese. But be careful as these two terms are not synonymous.
Overweight and obesity are two categories defined by specific values of body mass index (BMI). BMI equals a person's weight in kilograms divided by their height in metres squared.
For example, The BMI of a person weighing 83 kg and measuring 1.75 metres is equal to:
83 ÷ (1.752)2 = 83 ÷ 3.0625 = 27.10
By definition, a person with a BMI above 25 is considered to be overweight. We talk about overweight when the BMI is between 25 and 29.9 and obesity when the BMI is equal to or greater than 30.
Why is there currently talk of an "epidemic" of obesity?
The term "epidemic" is not restricted to infectious diseases: it means a sudden increase in the frequency of a disease or risk factors (like obesity) that are detrimental to health. We have been witnessing a steady increase in the number of overweight or openly obese people for a good ten years now and this applies throughout the world.
What are the causes of this epidemic?
The increase in the frequency of obesity is an adverse consequence of current lifestyles. Many of us have a diet too high in calories but also containing too much sugar and animal fat. This results in storage of excess absorbed energy in the form of adipose tissue. Another very important factor responsible for obesity is physical inactivity, that is to say the lack of physical exercise facilitated by modern conveniences: cars, lifts and escalators, not to mention long hours spent in front of the TV or computer. The imbalance between too much energy intake and reduced energy expenditure is an infallible recipe for promoting obesity.
Being overweight promotes the development of osteoarthritis
What are the risks associated with being overweight or obesity,
especially among people with osteoarthritis?

Numerous studies on this subject show that excess weight promotes osteoarthritis and aggravates its evolution. It is estimated that the risk of knee osteoarthritis is four times higher in obese women and 5 times higher among obese men than among the same sex but of normal weight. An increased risk of osteoarthritis of the hip associated with excess weight, certainly lower than for the knee, has also been proven. Thus, total hip replacements are 2.5 times more common in men with moderate obesity and over two thirds of patients undergoing surgery for hip osteoarthritis are overweight.
Also, one should bear in mind that, in patients with or without osteoarthritis, simply being "a bit plump" (overweight) or significantly "too fat" (obesity) causes metabolic disturbances that increase the risk of chronic diseases such as hypertension and type 2 diabetes and even myocardial infarction or stroke. In other words, there is more than one good reason to reduce even moderate excess weight because any weight loss can have significant benefits in terms of health.
Why does excess weight promote the development of osteoarthritis?
It is obvious that being overweight has negative consequences for weight-bearing joints such as vertebrae, hips and knees.
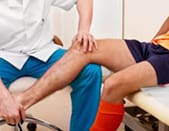
For example, the knees are subjected to a force equal to 3 to 6 times the body weight when walking. It is therefore not surprising that we have been able to show a connection between cartilage breakdown and the increase in load due to obesity.
Beyond this purely mechanical effect, other factors related to excess weight may promote osteoarthritis. Indeed, osteoarthritis of the hand is more common in overweight people than in people of normal weight. The role of a metabolic factor, leptin, secreted by the adipose tissue but also by the cartilage cells, could play a role but this is still only a hypothesis.
Obesity increases stress on the weight-bearing joints such as the hips.
Eating better ... and getting more exercise!
Excess weight is promoted by lack of exercise. But does exercise risk worsening osteoarthritis by overloading the joints even more?
Some physical exertion is contraindicated, but avoiding all forms of exercise to go easy on your joints would be a mistake.
It is actually recommended to do suitable exercises depending on the site, symptoms and stage of development of your osteoarthritis, but also based on whether you have any other health problems such as, for example, heart disease. This notion of suitability is essential and your doctor will be able to determine an individual programme with you, possibly with the help of a physiotherapist.
In people with osteoarthritis, the beneficial effects of regular exercise are not limited to weight loss or maintaining a normal weight. One can also expect a decrease in pain and stiffness of joints and even a slowing down in the progression of osteoarthritis. Exercise strengthens the muscles that support the joints which helps them to better withstand the weight they have to bear. Continued efforts also improve joint flexibility.
Do you need to follow a special diet to regain a normal weight when you have osteoarthritis?
No. The dietary principles are the same as for anyone who is overweight: reduce the consumption of red meats and sausages in favour of white meat and fish, reduce refined sugars in favour of carbohydrates and increase the quantities of fruit vegetables, cereals and pulses. Advice from a specialist in dietetics and monitoring changes in eating habits can be very useful.
Even moderate weight loss can improve your quality of life
In practice, how should you lose weight to get relief of the symptoms of osteoarthritis?
A study published in 2004 enables answering this question very precisely.
More than 300 subjects aged at least 60 years, all having excess weight (BMI greater than or equal to 28 kg/m2) with painful knee osteoarthritis proven radiologically were divided into four groups:
- Advice for a healthier lifestyle;
- Diet (calorie reduction and change in the composition of meals);
- Exercise (aerobic and resistance exercises for an hour three times a week);
- Diet plus exercise.
In this study lasting 18 months, called ADAPT (Arthritis, Diet and Activity Promotion Trial), subjects in the diet plus exercise group lost an average of 5.7% of their body weight. The study showed that moderate weight loss corresponded to an improvement in physical function by 24% (assessed by the subjects themselves but also demonstrated by specific measurement scales measuring the time spent on climbing stairs or the distance walked in 6 minutes) and a decrease in pain of more than 30%.
These improvements began to occur after 6 months and persisted until the end of the study, that is to say, during the following 12 months.
Losing 5-6% of body weight is a realistic, easy to achieve goal for most subjects, and this modest weight loss can lead to very significant improvements.
Reference:
- Messier SP, Loeser RF, Miller GD, et al. Exercise and dietary weight loss in overweight and obese older adults with knee osteoarthritis: the Arthritis, Diet, and Activity Promotion Trial. Arthritis Rheum 2004;50:1501-10.