What are they used for
Prostheses replace joints that are very damaged by osteoarthritis by joints in synthetic materials. The indication is never urgent because it is, before all else, for improving comfort. The decision for surgery is made jointly by yourself, your doctor and the surgeon.
They generally give good results with a reduction in the pain associated with osteoarthritis and a satisfactory return to mobility. However, you need to keep in mind that a prosthetic joint rarely functions as well as a normal joint. The safest techniques with the best results are those currently used for the hip and knee.
How do they work ?

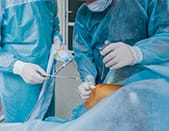
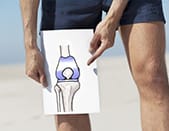
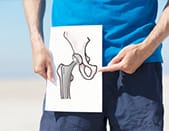
They are mainly joints of the knee and hip. The prostheses are made from various materials and attached to the bone with a special cement or "biological glue".
The procedure is carried out under general or loco-regional anaesthetic. It also involves an autologous blood transfusion, (collection of your blood before the procedure and reinfusion of it if necessary during the procedure). This technique removes the risk of a blood transfusion.
Hospitalisation lasts for about a week but is advisable to spend the following 4 to 6 weeks in a rehabilitation centre.
What precautions need to be taken ?
In all cases this type of surgery is only necessary if all the medical treatments have failed. The materials used have the disadvantage of becoming worn out after 15 to 20 years, and even faster in young and active people. This why complete joint replacement surgery is generally not proposed to people under the age of 55 to 60 years (except in special cases).
Preparation is required:
- Strengthening of the muscles that will surround the future prosthesis;
- Weight loss in the case of obesity;
- Elimination of any infection (teeth, sinuses, etc.)
Some surgeons recommend a delay of one or even several months between the last corticosteroid injection and the joint replacement surgery to be safe from a potential infection with the corticosteroids. The risks are those of any surgical procedure, but there are specific complications with regard to prostheses:
- The prosthesis can become detached from the bone on which it was attached: this is cement breakdown which can sometimes be of infectious origin (1 to 2%);
- Bad positioning of the prosthesis;
- And less serious, problems with muscular or tendon pain that disappears after correct rehabilitation.