Osteoarthritis is a chronic, slowly evolving disease leading to pain and sometimes to functional impairment and disablement. It can have a strong impact on your quality of life, be it your professional, social or family life.
It corresponds to a gradual deterioration of the different joint components under the effect of various factors of varying significance. While some factors, such as age and genetic predisposition, cannot be modified, there are others on which you can act to delay the onset of osteoarthritis and stop it from evolving. Get informed, talk to your doctor and you will see that osteoarthritis is not inevitable!
To prevent osteoarthritis and its complications, it is essential to fight against the main risk factors which are those of being overweight, joint injury, repeated micro-trauma and various lower limb abnormalities.
Is there a link between lower limb abnormalities and osteoarthritis?
Some lower limb abnormalities can promote the onset of osteoarthritis. Thus, congenital dysplasia of the hip is a known risk factor of osteoarthritis of the hip. With regard to the knee, studies have shown that there are more cases of knock-knee (valgus deformation) in patients with osteoarthritis than in normal patients. However, it is not known whether osteoarthritis of the knee is the cause or the consequence of knock-knee. On the other hand, we know that these abnormalities promote the progression of osteoarthritis.
In practice: how can these abnormalities be corrected?
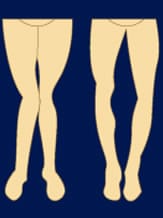
If you have a joint abnormality and already suffer from osteoarthritis with radiologic signs, even minimal, a surgical procedure may eventually be proposed to you.
The most frequent is osteotomy. It is carried out in the case of internal femorotibial osteoarthritis when there is deformation of the knee in genu varum (bow-leggedness).
This procedure involves cutting the upper section of the tibia, for removing or adding a bone "wedge" to shift the balance of the tibia towards the outside and thus shift the stress exerted on the damaged medial femorotibial compartment towards the healthy lateral femorotibial compartment. It does not touch the knee joint as such.
It offers you relief for several years and delays or prevents the need for a prosthetic knee joint.
What activities are best avoided?
A relatively mild but regularly repeated traumatism can promote the onset and worsening of osteoarthritis.
Hence, carrying heavy loads, working in a crouched or kneeling position or even using power tools such as pneumatic drills or chisels on a frequent basis promotes the onset of osteoarthritis of the spine, knee, elbow and hip.
In the same way, some top-level sportsmen or women who put a lot of strain on their joints develop osteoarthritis more easily: osteoarthritis of the hip in footballers, rugby players and dancers, osteoarthritis of the elbow in javelin throwers, osteoarthritis of the feet in dancers, osteoarthritis of the fingers in judokas.
In practice: which activities can promote the onset of osteoarthritis?
Professional activities which provoke or maintain pain must be temporarily or definitively stopped. In some cases, a job reclassification may be necessary (see the article on Osteoarthritis and work).
Even if you do not have osteoarthritis, beware of practising a sport in an intensive and prolonged way!
If you suffer from osteoarthritis it is advisable to maintain a moderate and regular exercise routine, eventually including a sport. In the event of osteoarthritis of the hip and/or knee, you can pursue sports activities that do not require sudden effort such as swimming, cycling or even jogging on condition of doing it on loose soil and with good quality running shoes. Any sport that makes joint pain worse or leads to synovial effusion (tenderness and swelling) should be avoided!
Why should any joint injury be treated quickly and efficiently?
A serious joint traumatism responsible for injury to the cartilage is likely to lead to the future onset of osteoarthritis. This is the case, for example, in the classic “dashboard injury” during road accidents which is sometimes responsible for:
- Injury to the cartilaginous menisci of the patella;
- A fracture of the upper part of the tibia which sometimes leads to osteoarthritis of the knee;
- A fracture to the lower end of the leg bone which can lead to secondary osteoarthritis of the ankle.
While the x-ray of a bone fracture is often impressive, bone usually heals completely, to the contrary of cartilage.
In the same way, a severe traumatism causing injury close to the cartilage can lead to the future onset of osteoarthritis. This is notably the case for a serious knee sprain (affecting the cruciate ligaments of the knee) or ankle sprain, but also for a tear and, in particular, a meniscal ablation.
If you undergo a surgical or arthroscopic meniscal ablation, you need to be aware that this can lead to osteoarthritis of the knee and, even more so, if the meniscus is completely removed and you suffer from genu varum (bowed legs). In this case, avoid any intensive high-risk sport!
In all cases, do not neglect any joint traumatism, in particular sprains!
Does losing weight enable limiting the risk of osteoarthritis?
The answer is unquestionably YES as regards the knee joint.
Indeed, you need to be aware that:
- If you do not have osteoarthritis but have excess kilos, you have a higher risk of developing knee osteoarthritis at a later date;
- If you lose your excess kilos, even only partially, you will reduce this risk;
- If you suffer from knee osteoarthritis and have excess kilos, your condition will evolve more quickly than if your weight were normal;
- If you have osteoarthritis of the knee and excess kilos, you will reduce the risk of your osteoarthritis getting worse and reduce your pain by losing weight.
Obesity increases the mechanical stress to the knee joint. It can be assessed by your body mass index (BMI):
- A BMI higher than 27, increases the risk of knee osteoarthritis by 14% with each increase of one kg/m2;
- A BMI of 30 multiplies the risk of knee osteoarthritis by 8;
- A BMI higher than 36 multiplies the risk of knee osteoarthritis by 13.
But obesity also promotes osteoarthritis of the fingers, probably by means of inflammatory mechanisms.
In practice: how do you calculate your BMI?
The body mass index (BMI) enables estimating the amount of excess fat in the body to define corpulence. The higher the BMI is, the higher risks associated with obesity become.
To calculate your BMI, you simply need to divide your weight (in kg) by your height squared (in m):
BMI (kg/m2) = Weight (kg)/height (m) x height (m).
To determine your corpulence, consult the body mass index table by clicking on the link >> Here
Is it necessary to take vitamins?
A balanced supply of vitamins C, D and E is recommended as part of a balanced diet, but at the moment there is no scientific proof to back-up that a dietary supplement (with tablets) is beneficial for people suffering from osteoarthritis.
Is hormonal treatment indicated?
Osteoarthritis of the knee appears more frequently in women after the menopause than in men.
The cause: the drop in oestrogenic hormone levels, which speeds up the deterioration of the cartilage. Hormonal replacement therapy prescribed in the absence of any contraindication, to prevent osteoporosis may also contribute to preventing the onset of osteoarthritis. It would appear that osteoarthritis of the hip is observed less frequently in women who have received or are receiving hormone replacement therapy.
In the event of existing osteoarthritis there is no scientific argument to believe that such a treatment could have an effect on its progression.
Lastly, remember: to prevent your osteoarthritis from getting worse, follow the medical or non-medical treatment prescribed by your doctor together with his or her advice!