Osteoarthritis is a disease of the cartilage. The latter is effectively the primary articular structure damaged by osteoarthritis. But other components also suffer the consequences as you will see in the rest of the chapter.
How is the cartilage damaged?
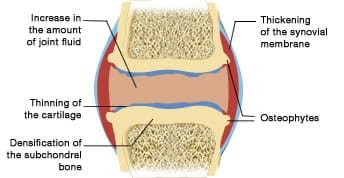
Osteoarthritis occurs following mechanical and biological phenomena and produces an imbalance between the production and the destruction of cartilage. This becomes predominant and lesions appear within the cartilage. This is commonly called "chondropathy" (chondro = cartilage and pathy = disease).
The cartilage will try to repair these lesions, but will gradually become incapable of compensating for the imbalance.
The thickness of the cartilage diminishes leading to narrowed joint space (the two ends of the bones get closer together) and fissures appear in the cartilaginous tissue. They may extend right up to the subchondral bone. The latter becomes condensed in reaction to the narrowed joint space. Following the same principle, a bony proliferation may occur pushing the cartilage towards the outside of the joint, leading to the appearance of osteophytes.
Lastly, the synovial membrane also plays a significant role in osteoarthritis. The deterioration of the cartilage releases substances in the joint which irritate the synovial membrane.
- The latter thus produces synovial fluid in a greater quantity which leads to the build up of excess synovial fluid and the classic “synovial effusion”.
- This liquid is also of not such good quality as the normal liquid with a weaker concentration of hyaluronic acid. It does not protect the cartilage as well as it should and this contributes to the damage of the latter.
How do we see this in an x-ray?
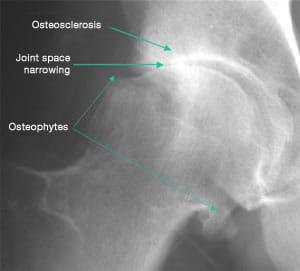
Osteoarthritis is confirmed by x-rays that your doctor may need to request.
If the cartilage is invisible on the x-ray the indirect signs enable confirming the presence of osteoarthritis:
- a reduction in the height of the cartilage indicates narrowed joint space, which means that the space between the ends of the two bones is diminishing;
- the subchondral bone reaction which becomes condensed appears on the x-ray as “whiter-looking” than the bone;
- lastly, the osteophytes manifest themselves as bony projections that are visible along the outline of the joint.
It is important to understand that there is not always a concordance with the amount of lesions visible on the x-ray and the signs that are actually felt:
- some patients are in a lot of pain with few signs on their x-ray
- while others are able to tolerate their osteoarthritis in spite of impressive x-ray images.
Why is osteoarthritis so painful?
Cartilage does not have a nerve network. So this is not what hurts in osteoarthritis. Indeed the pain that is felt comes from neighbouring tissues that are also affected by the osteoarthritis lesions: the synovial membrane in particular, but also the subchondral bone, the ligaments and the tendons.
The pain information begins in the nerve endings present in these tissues. It follows the nerve network right up to the spinal cord and finally reaches the brain which triggers the sensation of pain.
It is also worth noting that once the cartilage is damaged, a "neo-neurogenesis" may occur. This means the appearance of nerve endings within the cartilage which initially did not have any because of the osteoarthritis.
Is arthritis an age-related disease?
Osteoarthritis is not synonymous with ageing. They are effectively two different mechanisms even though they are often associated with one another: osteoarthritis is a real disease and not the inevitable effect of ageing.
Ageing alone is not sufficient to bring about the onset of osteoarthritis. However, it is certain that it is responsible for the cartilage having less resistance to various injuries and thus promotes the onset of osteoarthritis.
Everything occurs as if osteoarthritis were an exaggerated caricature and acceleration of the phenomena encountered during the ageing process.